
Patients want to know what they owe. You want to get paid quickly. Checking patients’ eligibility before and at the time of service helps solve both problems by reducing the need for future statements and collection follow-up. It also helps prevent costly claim rejections and denials.
But what is the best way to obtain up-to-date dental insurance information? Utilize automated technology that is integrated within your practice management system. There are third-party companies that offer insurance verification solutions, but only a few are integrated with Open Dental. Integration creates a unified experience by eliminating the need to work outside of Open Dental to manually call payers, visit web portals, or log into different systems to manage inquiries. With just a few clicks, you get instant access to comprehensive eligibility information like plan benefits, deductibles, co-insurance, limitations, and more from hundreds of payers.
Beyond ease of use, electronically checking eligibility creates tangible results, including:
- Cost savings – an average of $5.63 is saved per transaction compared to manual methods.*
- Time savings – dental practices can save an average of 10 minutes per transaction.*
- Patient satisfaction – communicate treatment cost estimates and payment responsibilities at the time of service.
Integrated Eligibility with Open Dental is Easy
Ready to stop chasing information from multiple payer sites, but not quite sure how to get started? Don’t worry. DentalXChange is an integrated verification option. The steps are outlined below, along with a few tips and tricks to help your practice incorporate this solution into your workflow.
Once you’ve signed up with an integrated Clearinghouse for eligibility, set it in Setup, Clearinghouses by clicking the Eligibility button. If this is a different Clearinghouse than you use to send claims, double-click to enter any account details as well.
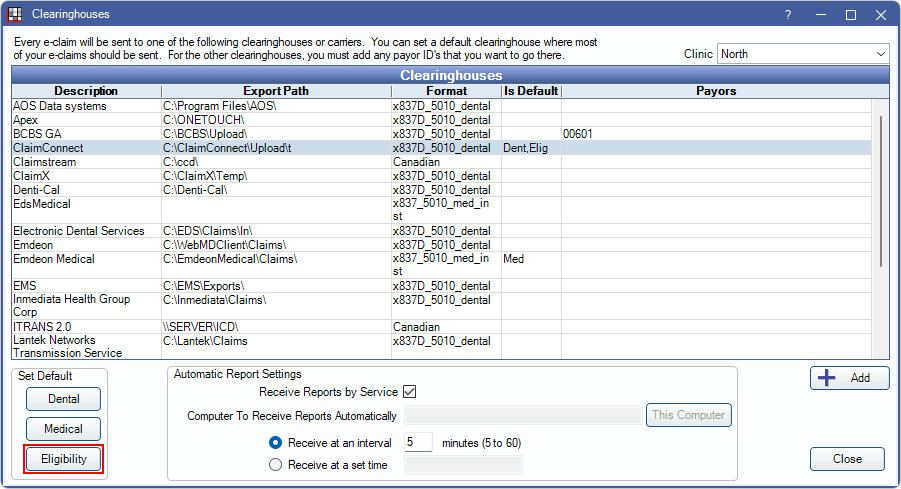
Now you’re ready to start requesting electronic benefits directly through Open Dental! There are two different places you can do this: the Insurance Verification List and the Edit Insurance Plan window.
Use the Insurance Verification List to verify eligibility and benefits for patients who have upcoming appointments. Easily view plan and subscriber information by selecting a patient or right-click to quickly open the insurance plan to verify benefits and request electronic benefits – all without leaving the window. The Insurance Verification List can also be open while you work in other modules, just in case you do need to leave the window.

If you’re adding a new insurance plan to a patient, have a new patient, or just need to verify benefits for a single patient, you can request electronic benefits in the Family Module. Just double-click the insurance plan and click the Request button.

Whether you get to the request from the Family Module or the Insurance Verification List the steps to import will be the same. The response you get will depend on the payer. Some may provide detailed benefit information, while others may not.
Compare the Response Benefit Information with the Current Benefits. If something is already entered in the Current Benefits, it doesn’t need to be imported (you’ve already entered it). Highlight the benefits you do want to import and click Import. This information is now added to your insurance plan.

Once you’ve verified your patient’s eligibility and benefits, update the Eligibility Last Verified and Benefits Last Verified dates as needed. If you’re in the Edit Insurance Plan Window, you can click the Now buttons next to these fields to insert today’s date.

From the Insurance Verification List, you can also, select a patient and use the Mark Patient Eligibility and Mark Ins Benefits Verified or right-click Verify Patient Eligibility and Verify Insurance Benefits to insert today’s dates into the Last Verified fields.

Instant verification. Instant gratification.
Make fine-tuning your insurance verification process a top priority. It has substantial cost and time-saving benefits and a significant impact on the patient experience. Setting up an integrated solution within Open Dental is simple, and the benefits are immediate.
As an integrated partner, Eligibility from DentalXChange provides a single source of truth. This solution offers instant access to 950+ in-network payers. DentalXChange continually grows payer connections and additional functionality to meet clients’ evolving eligibility data needs. This results in minimized data entry with a rich return of benefit information in a standardized display. Information is easy to understand and enables you to share patient out-of-pocket costs and reimbursements at time of service.
Ready to make Eligibility easier? Connect with a DentalXChange Payments Pro today. Visit DentalXChange or call 800.576.6412, ext. 455, to get started.
Since 1989, DentalXChange has been on the forefront of modernizing and innovating dental claims creating dental payment solutions that bring ease to the payments process. Today, it has grown to support a current client base of more than 107,000 dental providers. Headquartered in Irvine, CA, through its own clearinghouse, state of art technology consisting of modern APIs, and secure Web portals, DentalXChange processes over 300 million transactions, consisting of more than 71 million dental claims annually.
